
Chiari Malformation
Overview:
Chiari malformation happens when part of the lower brain sits too low and pushes into the spinal canal. This can block the flow of cerebrospinal fluid (CSF) and cause headaches, neck pain, and neurological symptoms. Some people are born with it and do not notice symptoms until later in life.
Common Symptoms:
- Headaches, often worse with coughing or straining
- Neck pain
- Balance problems or dizziness
- Numbness or tingling in the hands
- Trouble swallowing
- Ringing in the ears
Treatments & Procedures:
- MRI with CSF flow studies
- Chiari decompression surgery
- Duraplasty when needed to improve CSF flow
- Pain and symptom management for mild cases
- Monitoring when symptoms are stable
Congenital Brain and CSF Disorders
Congenital Brain and CSF Disorders
Overview:
Congenital brain and CSF disorders are conditions that are present at birth. These conditions affect brain development or the normal flow of CSF. Some are found before birth, while others are diagnosed in infancy or childhood.
Common Symptoms:
- Delayed development
- Enlarged head size in infants
- Seizures
- Weakness or muscle stiffness
- Feeding or breathing difficulties
Treatments & Procedures:
- Shunt placement or revision
- Endoscopic CSF procedures
- Corrective neurosurgery when needed
- Long-term monitoring and care
CSF Flow Obstruction
Overview:
CSF flow obstruction occurs when cerebrospinal fluid cannot move normally through the brain or spine. This blockage can raise pressure and cause symptoms. Obstruction may be caused by tumors, cysts, scarring, or structural changes in the brain or spine.
Common Symptoms:
- Headaches
- Nausea or vomiting
- Vision changes
- Balance problems
- Weakness or numbness
Treatments & Procedures:
- Endoscopic procedures to restore CSF flow
- Shunt placement
- Surgical removal of the blockage
- Imaging and pressure testing
Hydrocephalus
Overview:
Hydrocephalus happens when too much cerebrospinal fluid (CSF) builds up in the brain. This can increase pressure and affect how the brain works. It may be present at birth or develop later in life from injury, infection, bleeding, or a blockage in the CSF pathways.
Common Symptoms:
- Headaches or pressure
- Balance problems
- Nausea or vomiting
- Vision changes
- Trouble walking or thinking clearly
Treatments & Procedures:
- Ventriculoperitoneal (VP) shunt
- Ventriculoatrial (VA) or lumboperitoneal (LP) shunt
- Endoscopic Third Ventriculostomy (ETV)
- Shunt revisions or adjustments
- Monitoring with imaging or pressure studies
Normal Pressure Hydrocephalus
Normal Pressure Hydrocephalus
Overview:
Normal Pressure Hydrocephalus is a type of hydrocephalus that usually affects older adults. Even though pressure inside the head may look normal, too much cerebrospinal fluid (CSF) still affects brain function. It often causes changes in walking, thinking, and bladder control.
Common Symptoms:
- Shuffling or unsteady walk
- Memory or thinking problems
- Urinary urgency or incontinence
- Feeling slow or confused
Treatments & Procedures:
- Diagnostic tap test to check for improvement
- VP shunt placement
- Shunt adjustments to improve symptoms
- Ongoing monitoring with neurology and neurosurgery
Syringomyelia
Overview:
Syringomyelia is a condition where a fluid-filled cavity (called a syrinx) forms inside the spinal cord. It often develops from Chiari malformation but can also follow injury, infection, or spinal surgery. As the syrinx grows, it can damage nerves and affect movement and feeling.
Common Symptoms:
- Neck or back pain
- Weakness in the arms or hands
- Loss of feeling, especially temperature changes
- Stiffness in the arms or legs
- Worsening balance
Treatments & Procedures:
- MRI to monitor syrinx size
- Chiari decompression surgery (if the syrinx is caused by Chiari)
- Syrinx drainage or shunt (in select cases)
- Treatment of the underlying cause
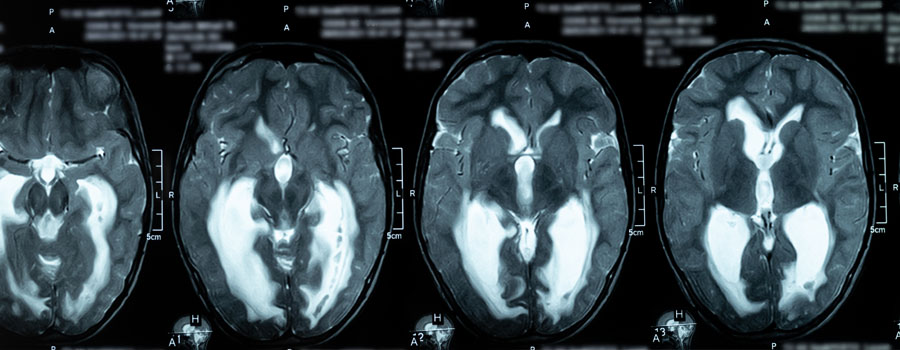
We've highlighted some of the most common services—please explore the conditions list for treatments by condition.
Advanced CSF Imaging and Diagnostic Testing
Advanced CSF Imaging and Diagnostic Testing
Overview:
MRI, CT, and CSF flow studies help identify blockages, pressure changes, or Chiari-related problems. These tests guide decisions about surgery or shunt placement.
Conditions Treated:
- Hydrocephalus
- Chiari malformation
- Syringomyelia
- CSF flow disorders
Before the Procedure:
Most imaging tests require no special preparation. Some MRIs may need contrast dye.
After the Procedure:
You can return to normal activity right away. Your care team will review results and discuss next steps.
Chiari Decompression Surgery
Chiari Decompression Surgery
Overview:
Chiari decompression reduces pressure at the base of the skull where the brain meets the spine. Removing a small amount of bone and, in some cases, opening the dura helps restore normal cerebrospinal fluid (CSF) flow and relieve symptoms.
Conditions Treated:
- Chiari Malformation Type I
- Chiari-related headaches and neck pain
- Chiari-related syringomyelia
Before the Procedure:
MRI with CSF flow studies helps plan the surgery. Your surgeon will explain the steps and discuss anesthesia and recovery. You may need to stop certain medicines ahead of time.
After the Procedure:
Most patients stay several days in the hospital. Neck soreness is common at first. As healing continues, headaches, balance problems, and other symptoms often improve. Follow-up imaging may be needed.
Endoscopic Third Ventriculostomy
Endoscopic Third Ventriculostomy
Overview:
Endoscopic third ventriculostomy (ETV) is a minimally invasive procedure that creates a new pathway in the brain to allow fluid to flow and relieve pressure. It’s often an alternative to shunt placement.
Conditions Treated:
- Hydrocephalus
- Blocked fluid pathways in the brain
Before the Procedure:
Children will need an MRI or other imaging to confirm they are a candidate for ETV. Instructions may include stopping food or drink before surgery.
After the Procedure:
Most children recover in the hospital for one or two days. Follow-up imaging helps confirm that fluid is draining properly and symptoms are improving.
Intracranial Pressure Monitoring
Intracranial Pressure Monitoring
Overview:
Intracranial Pressure Monitoring measures the pressure inside the skull using a small sensor. This helps diagnose pressure disorders or guide treatment for cerebrospinal fluid (CSF) flow problems.
Conditions Treated:
- Suspected CSF pressure disorders
- Hydrocephalus with unclear symptoms
- Conditions affecting brain swelling or fluid balance
Before the Procedure:
Imaging helps guide placement. The sensor is placed during a short procedure under anesthesia. Monitoring may continue for a day or longer.
After the Procedure:
You will remain in the hospital while the care team tracks pressure changes. The sensor is removed once testing is complete. Results guide your treatment plan.
Shunt Revision or Replacement
Shunt Revision or Replacement
Overview:
A shunt may need adjustments, repair, or replacement if it stops working as expected. Shunt revisions help keep cerebrospinal fluid (CSF) flowing properly and prevent symptoms from returning.
Conditions Treated:
- Shunt malfunction
- Blocked or infected shunts
- Symptoms returning after prior improvement
Before the Procedure:
Imaging and a full exam help identify the problem. You may need blood tests or pressure studies. Your surgeon will explain the plan and review anesthesia details.
After the Procedure:
Recovery is similar to the original shunt surgery. You will have follow-up visits to check healing and confirm that symptoms are improving again.
Syrinx Drainage or Shunting
Syrinx Drainage or Shunting
Overview:
When a syrinx (fluid-filled cavity in the spinal cord) causes symptoms, a small drainage tube or shunt may be placed to help fluid flow. This reduces pressure inside the spinal cord.
Conditions Treated:
- Syringomyelia
- Syrinx from Chiari malformation
- Syrinx from injury or infection
Before the Procedure:
Imaging is used to locate the syrinx and guide planning. Your care team will explain anesthesia, surgical steps, and expected recovery.
After the Procedure:
Neck or back soreness is common for a few days. Symptoms like weakness or numbness may improve over time as pressure decreases. Follow-up imaging checks the syrinx size and stability.
Ventriculoatrial (VA) and Lumboperitoneal (LP) Shunts
Ventriculoatrial (VA) and Lumboperitoneal (LP) Shunts
Overview:
VA and LP shunts are alternatives when a VP shunt is not the best option. A VA shunt drains fluid into a blood vessel in the neck. An LP shunt drains fluid from the lower spine into the abdomen.
Conditions Treated:
- Hydrocephalus
- NPH
- CSF buildup when other pathways cannot be used
Before the Procedure:
Imaging and lab tests help guide the decision. Your surgeon will explain which shunt type fits your needs. You will receive instructions about anesthesia and activity.
After the Procedure:
Most patients recover with simple wound care. Follow-up visits allow the team to adjust the shunt and check progress. Symptoms usually improve over time as pressure normalizes.
Ventriculoperitoneal Shunt
Ventriculoperitoneal Shunt
Overview:
A ventriculoperitoneal (VP) shunt is a small device that removes extra cerebrospinal fluid (CSF) from the brain and drains it into the abdomen, where the body absorbs it. This lowers pressure in the brain and helps improve symptoms of hydrocephalus.
Conditions Treated:
- Hydrocephalus
- Normal Pressure Hydrocephalus (NPH)
- CSF flow blockages
Before the Procedure:
You will have imaging tests such as MRI or CT to plan the surgery. Your care team will review medicines to stop before surgery and explain what to expect. Most patients receive general anesthesia.
After the Procedure:
You may stay in the hospital for monitoring. Some soreness near the incision is normal. A programmable shunt may be adjusted in follow-up visits to find the best setting. Most people notice gradual improvement in walking, balance, or thinking.
Can’t find what you're looking for? Contact the care team at the clinic for assistance.