Reba Smith-Weeden’s hand shook so bad, she couldn’t drink a cup of coffee. She has a condition called essential tremor that prevented her from carving the Thanksgiving turkey one year at her Kemah home.
“I couldn’t do it,” she said.
Essential tremor is a neurological condition that is 10 times more frequent than Parkinson’s disease. It is an involuntary tremor that can happen as someone tries to do an everyday, normal movement, such as trying to pick up and hold a cup of coffee.
Smith-Weeden, 67, first noticed some shaking when she was in her 40s. At the time, she attributed it to being hungry or anxious. It got worse over 25 years. For the last four years, the shaking has been a major issue in her life.
“It was just a little bit of shaking in the beginning, but it slowly got worse,” Smith said. “I couldn’t do normal things.” 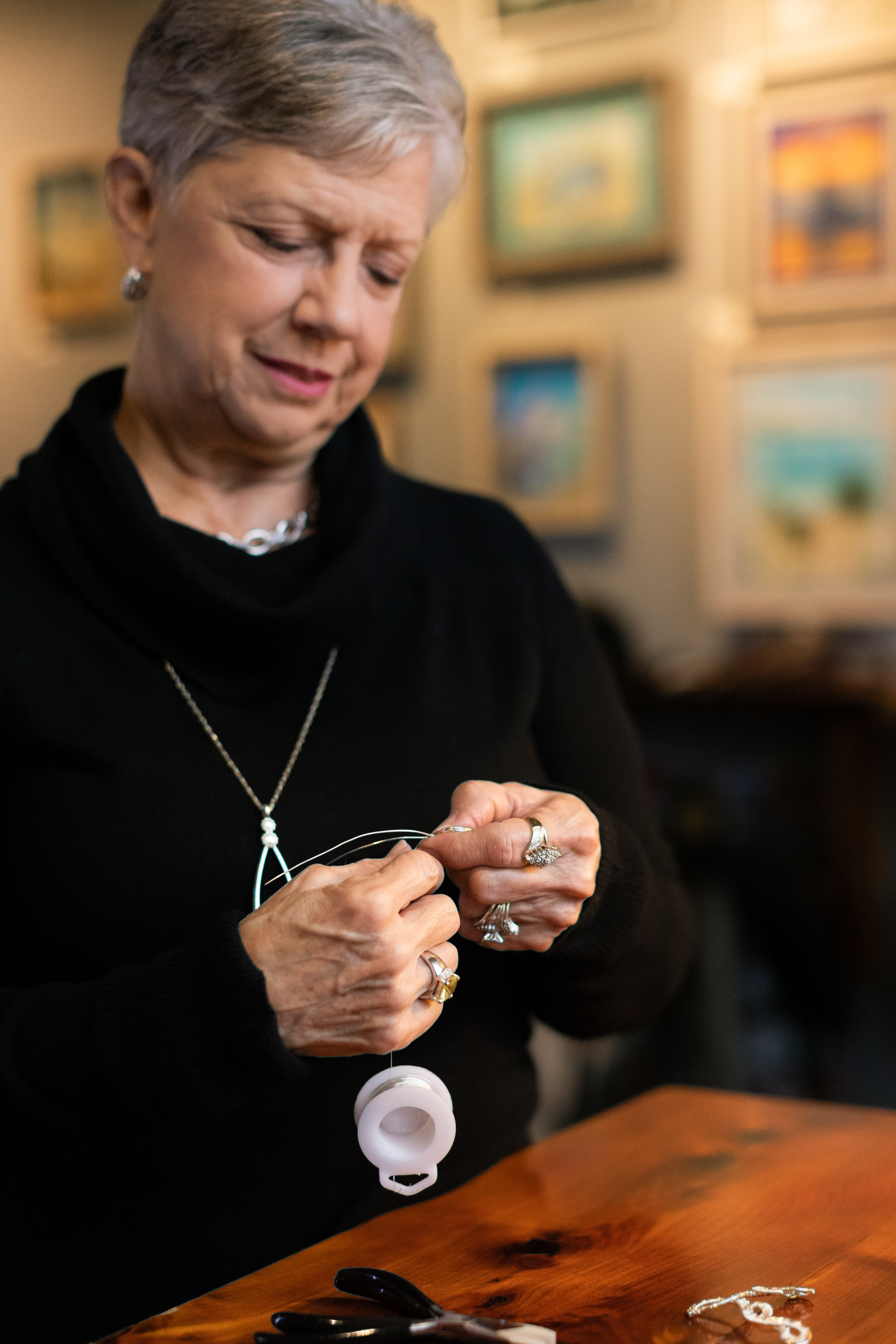
She couldn’t write her own name with her dominant hand. She learned to write it with her left, even though she still struggled with the shaking as she did it.
She used to make jewelry out of pieces of sea glass she collected in Mexico. She would wrap and weave wire around the sea glass to create jewelry. “I haven’t been able to do that,” she said.
Smith-Weeden started seeing a neurologist and tried a number of different medications. “Nothing seemed to work,” she said. “I was still shaking.”
A solution
Her doctor suggested she consider deep brain stimulation, often abbreviated DBS, a two-part operation that allows electrical stimulation to the brain.
Curious, Smith-Weeden began her research. She found a video online of a man who had the same type of surgery.
“He was still on the table, and they gave him a violin and he could play,” she said. “I was just like, wow! He wasn’t shaking. And he played it beautifully.”
A small mechanism turned the electrical stimulation on. She was convinced.
She met Dr. Patrick Karas, a neurosurgeon, who had just joined UTMB and performed deep brain stimulation.
“He made me feel at ease,” Smith-Weeden said. “He has a good bedside manner.”
The deep brain stimulation procedure involved two operations. The first surgery implants the electrodes in the brain. The second operation connects the electrodes to a pacemaker-type device in the chest.
Smith-Weeden had her first surgery in January and the second in February. Karas told her the device would be turned on one month after the initial surgery, but the shaking would stop immediately when the device is turned on.
The outcome
She remembers the day the shaking stopped. She had a follow-up appointment to test the device and how it was signaling her brain. The staff turned on the neurotransmitter.
Then her head stopped shaking and her voice tremors disappeared.
“They noticed it first before I did,” Smith-Weeden said. “I just cried. They programmed my neurotransmitter to tell my brain to stop shaking.”
They asked her to draw a spiral, and she did. She tried signing her name, and she could.
Now, she can put on her make-up. She can handcraft jewelry again. And she smiles a lot.
“I can drink my coffee without spilling it, I can eat without shaking, and I can brush my teeth.” Smith-Weeden said.
“This is life changing.”